Open Access | Case Report
This work is licensed under a Creative Commons Attribution-ShareAlike 4.0 International License.
Konno-rastan procedure combined with manougian root enlargement for small aortic root
*Corresponding author: Metin Onur Beyaz
Mailing address: Department of Cardiovascular Surgery, Faculty
of Medicine, Istanbul Medipol University, Medipol Mega University Hospital, TEM Avrupa Otoyolu Goztepe Cikisi, No:1, 34214 Bagcilar, Istanbul, Turkey
Email: metinonurbeyaz@gmail.com
11 October 2020 / Accepted: 30 November 2020
DOI: 10.31491/CSRC.2020.12.065
Abstract
Aortic stenosis is a rarely seen condition in the pediatric population. Valve replacement is a treatment option for patients who do not benefit from medical or interventional procedures. In this report, we described our surgical treatment strategy in a 17-year-old patient who developed patient-prosthesis mismatch long after initial aortic valve replacement during the childhood period.
Keywords
Konno-rastan procedure; manouguian technique; aortic root enlargement
Introduction
Aortic stenosis is a rarely seen condition in the pediatric
population. The known incidence is 3.8/10.000 in live
births [1]. Balloon angioplasty is the most common treatment method in the neonatal period for aortic stenosis
[2]. Valve replacement is another treatment option for
patients who do not benefit from medical and interventional procedures [3]. Valve replacement options include
Ross technique, Konno technique, and biological or
mechanical valve replacement. As the patients grow, patient prosthesis mismatch still appears as an important
factor who underwent valve replacement surgery [4].
In this report, we described the surgical treatment of a
17-year-old patient who developed patient-prosthesis
mismatch due to aortic valve replacement history.
Case Report
A 17-year-old male patient was admitted to our clinic
with complaints of increased chest pain and shortness of breath after exercise who underwent aortic
valve replacement surgery with a No: 17 mechanical
aortic valve with Manouguian aortic root enlargement
technique due to diagnosis of aortic stenosis 10 years
ago.
There was no family history. All biochemical markers
found normal. The cardiothoracic index was increased
in his chest x-ray. The patient was overweight with a
body mass index of 27.19 kg/m2
. Echocardiography
showed intact mechanical valve prosthesis with low
effective orifice area (Indexed EoA: 0.70) and ventricular hypertrophy. The ejection fraction was measured
at 55%. A mean transaortic pressure gradient was
measured 24 mmHg with a maximal aortic velocity of
3.4 m/s. Additionally, there was mild pulmonary insufficiency and stenosis, and mild mitral insufficiency.
Aortic valve replacement surgery was planned after
the patient and his family was informed about the operation and the necessary operation consent was obtained.
Surgical technique
Sternotomy incision was made along the old sternotomy incision line. Adhesions were removed. The pericardium was opened and suspended. Aortic cannulation and bicaval venous cannulations were performed
following systemic heparinization. Cardiopulmonary
bypass was initiated and the patient was cooled down
to 28 C. A vent catheter was inserted into the left atrium from the right superior pulmonary vein. Cardiac
arrest and myocardial protection were provided with
direct cold blood cardioplegia after aortic clamp and
aortotomy. The old aortic valve was excised. The pericardium used for the old Manougian procedure was
found to be calcified and resected. The right ventricle
outflow tract (RVOT) was opened and an incision was
extended to the interventricular septum. The septum
and the anterior aortic root was enlarged with a dacron
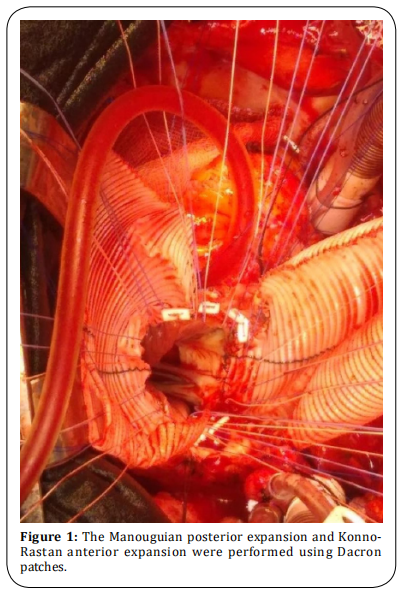
patch (Konno-Rastan procedure). The Manougian type
posterior enlargement was made with a dacron patch
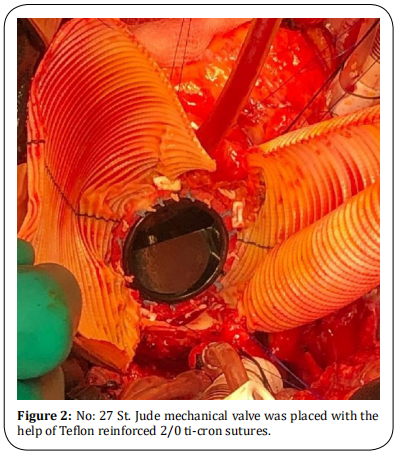
(Figure 1). No: 27 mechanical valve was implanted to
the aortic root with the help of Teflon reinforced 2/0
ti-cron sutures (Figure 2). The aortotomy was closed
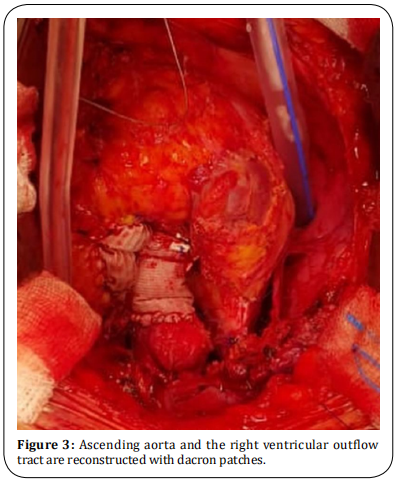
using a dacron patch. Pulmonary comissurotomy was performed to relieve mild pulmonary stenosis. RVOT
was reconstructed using a dacron patch (Figure 3).
Weaning of the cardiopulmonary bypass was achieved
with milrinone (0.75 mcg/kg/min) and adrenalin (0.05
mcg/kg/min) infusion. The operation was ended conventionally. The patient was taken to the intensive care
unit. The cardiopulmonary bypass and cross-clamp
times were 138 minutes and 106 minutes, respectively.
The patient was extubated in the 6th hour. The intensive care unit stay was 56 hours. Postoperative course
was uneventful and the patient was discharged from
the hospital after 8 days.
Postoperative echocardiography indicated no significant transaortic gradient (max: 4-5 mmHg) with normal myocardial functions. She has been followed active,
well, and asymptomatic for more than 18 months.
Discussion
Causes of aortic stenosis vary from congenital bicuspid aortic valve, calcification to rheumatic fever [5]. Untreated aortic stenosis has a classical triad composed of dyspnea, syncope and angina. Heart failure and rhythm disorders may be added to these symptoms in later stages [6]. PPM should always be avoided as it has been associated with perioperative mortality, reduced longterm survival, consistent symptoms, and slow regression of LV mass. Meta-analysis has reported that severe PPM is associated with reduced long-term survival [7]. Patient-prosthesis incompatibility is one of the problems affecting the quality of life of patients after aortic valve replacement surgery and this situation may be more prominent especially in children as their growth continue [8]. It has been shown that aortic root enlargement operations can be performed to overcome PPM, and the incidence of PPM is reduced with root enlargement operations. Konno-Rastan and Manouguian procedures are the two most commonly preferred root augmentation operations for patients. When KonnoRastan and Manouguian type aortic enlargement were together performed, it is possible to implant larger aortic valves to the aortic root especially in the growing population [9]. The Ross procedure is another option and by its nature, the patient’s pulmonary autograft is used to replace the aortic valve [10]. Ross procedure could have been an alternative; however, our patient was not found suitable for Ross procedure ten years ago due to having a bicuspid pulmonary valve showing mild pulmonary insufficiency and minimally fibrotic leaflets. A No: 17 mechanical valve could be implanted following posterior aortic root enlargement at that age. As the child grew up in time, this mechanical valve remained small as expected. What needs to be done in the meantime was to replace the valve.
Conclusion
A cardiac surgeon should be well skilled with the root enlargement procedures which may be helpful at the time of aortic valve replacement for young obese men and women with small aortic roots. Combined aortic root enlargement techniques could be considered in the presence of bodily growth potential.
Declarations
Authors’ contributions
Made substantial contributions to conception and design of the study and performed data analysis and interpretation: Beyaz MO, Elipek NG, Demir I, Oztas DM,
Ulukan MO, Ugurlucan M, Turkoglu H.
Performed data acquisition, as well as provided administrative, technical, and material support: Ugurlucan M,
Turkoglu H, Ulukan MO.
Availability of Data and Materials
All data of the patients are stored at Medipol University where the operations are performed.
Conflict of interest
All authors declared that there are no conflicts of interest.
Ethical approval
We studied in accordance with the ethical guidelines set by the Helsinki Declaration and the International Association of Heart and Lung Transplantation (ISHLT). A case report was prepared after obtaining a signed document and approval from the patient and his family for procedures.
References
1. Olofsson, C. K., Hanseus, K., Ramgren, J. J., Synnergren, M. J.,
& Sunnegårdh, J. (2020). A national study of the outcome
after treatment of critical aortic stenosis in the neonate.
Cardiology in the Young, 30(9), 1321-1327.
2. Nişli, K., Serra Karaca, D., & Dindar, A. (2016). Yenidoğanda
umblikal ven yoluyla aort balon valvüloplastisi: Ülkemizdeki ilk tecrübe. Turk Kardiyol Dern Ars, 44(6), 521-523.
3. San Román, J. A., Vilacosta, I., Antunes, M. J., Iung, B., Lopez, J., & Schäfers, H. J. (2020). The ‘wait for symptoms’
strategy in asymptomatic severe aortic stenosis. Heart,
106(23), 1792-1797.
4. Kim, H. J., Kim, H. J., Kim, J. B., Jung, S. H., Choo, S. J., Chung, C.
H., & Lee, J. W. (2020). Prosthesis-patient mismatch after
surgical aortic valve replacement in patients with aortic
stenosis. Interactive CardioVascular and Thoracic Surgery,
31(2), 152-157.
5. Maganti, K., Rigolin, V.H, Sarano, M.E, Bonow, R.O. (2009).
Valvular heart disease: diagnosis and management. MayoClin Proc, 85(5):483-500.
6. Minners, J., Rossebo, A., Chambers, J. B., Gohlke-Baerwolf,
C., Neumann, F. J., Wachtell, K., & Jander, N. (2020). Sudden
cardiac death in asymptomatic patients with aortic stenosis. Heart, 106(21), 1646-1650.
7. Head, S. J., Mokhles, M. M., Osnabrugge, R. L., Pibarot, P.,
Mack, M. J., Takkenberg, J. J., ... & Kappetein, A. P. (2012).
The impact of prosthesis–patient mismatch on longterm survival after aortic valve replacement: a systematic
review and meta-analysis of 34 observational studies
comprising 27 186 patients with 133 141 patient-years.
European heart journal, 33(12), 1518-1529.
8. Nardi, P., Russo, M., Saitto, G., & Ruvolo, G. (2018). Theprognostic significance of patient-prosthesis mismatch
after aortic valve replacement. The Korean Journal of Thoracic and Cardiovascular Surgery, 51(3), 161.
9. Khan, F. W., & Said, S. M. (2019). Konno-rastan combined
with manougiaun root enlargement for small aortic root
with coronary anomaly in a young woman. Heart Views:
The Official Journal of the Gulf Heart Association, 20(4),
172.
10. Erek, E., Kenan Yalcinbas, Y., Sarioglu, A., & Sarioglu, T.
(2004). Double root re-replacement after Ross–Konno
operation in a patient with straight back syndrome: clamshell approach. Interactive cardiovascular and thoracic
surgery, 3(4), 575-577.